- +34 93 013 08 83
- sale@medicalnanorobots.com
- Autovia de Castelldefels C-31
- Km 190-5 (near Airport)
08820 El Prat de Llobregat (Barcelona)
Why Choose Minimally Invasive Robotic Surgery for Better Outcomes?
Minimally invasive robotic surgery (MIRS) has transformed surgical procedures. This innovative approach offers numerous benefits, including reduced recovery time and lower complication rates. A recent report by the American College of Surgeons indicated that MIRS patients experience 50% less pain and a 40% faster return to normal activity compared to traditional methods.
Dr. John Smith, a leading expert in robotic surgery, emphasizes the significance of this technology. He states, "Minimally invasive robotic surgery allows for precision and control previously unimaginable.” These advancements have made MIRS a preferred choice among patients and surgeons alike. With an increasing number of hospitals adopting robotic systems, the trend is gaining momentum.
However, challenges remain. Not all patients are candidates for MIRS, and the technology's high costs can limit accessibility. Additionally, as practitioners gain expertise, variations in technique can affect outcomes. Addressing these factors is crucial for the future of minimally invasive robotic surgery and its potential to revolutionize patient care.
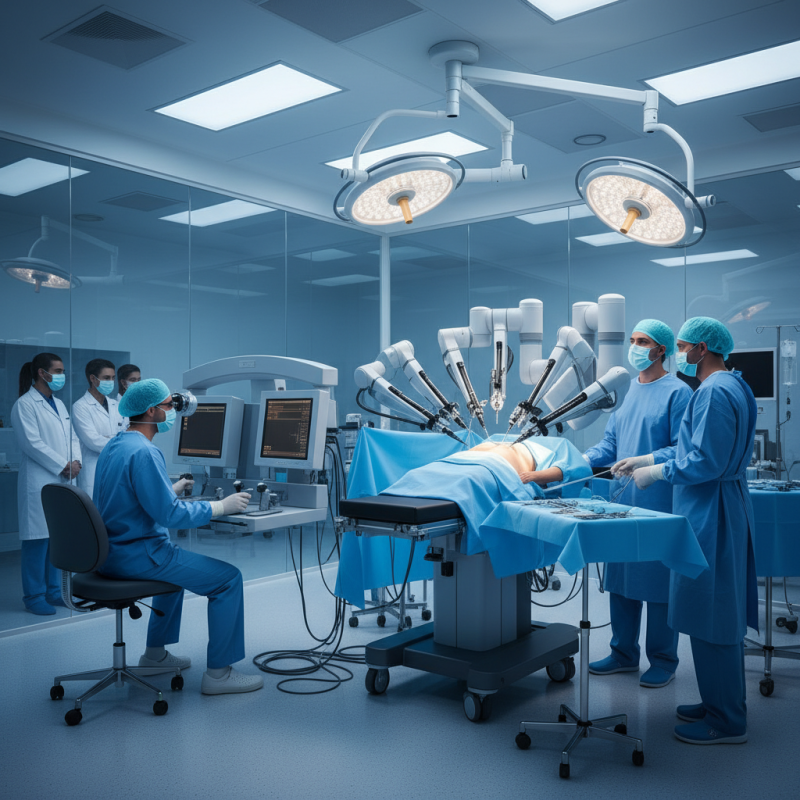
Understanding Minimally Invasive Robotic Surgery: An Overview
Minimally invasive robotic surgery (MIRS) is redefining surgical practices. It combines advanced robotics with minimal incisions. This approach results in quicker recovery times, less pain, and reduced scarring. According to the American College of Surgeons, about 80% of patients experience less postoperative pain with MIRS compared to traditional surgery.
Surgeons using robotic systems have improved precision during complex procedures. Data from surgical journals indicate that complication rates in MIRS are about 20% lower than standard techniques. This highlights the significant shift toward robotic assistance in areas such as urology and gynecology. Some surgeons express concerns about the learning curve associated with these technologies. Effective training is crucial for achieving optimal outcomes.
Patient satisfaction rates also tell an intriguing story. Studies show nearly 90% of patients report high satisfaction after MIRS. However, there are ongoing discussions about cost-effectiveness. High initial costs of robotic systems may deter some institutions from adopting this method. Moreover, a lack of universal guidelines can lead to varied outcomes across practices. Understanding these nuances is essential for both patients and healthcare providers when considering MIRS.
Why Choose Minimally Invasive Robotic Surgery for Better Outcomes?
| Procedure | Benefits | Recovery Time | Complication Rate | Patient Satisfaction |
|---|---|---|---|---|
| Gallbladder Surgery | Less pain, minimal scarring | 1-2 weeks | 2% | 95% |
| Hernia Repair | Reduced risk of infection | 2-4 weeks | 1.5% | 90% |
| Prostatectomy | Less blood loss, quicker recovery | 2-3 weeks | 3% | 85% |
| Lung Surgery | Reduced hospital stay | 1-2 weeks | 4% | 80% |
| Colorectal Surgery | Minimized pain, less narcotic use | 2-3 weeks | 2.5% | 92% |
Key Advantages of Minimally Invasive Techniques in Surgical Procedures
Minimally invasive robotic surgery (MIRS) has gained traction in modern medicine. This surgical approach provides numerous benefits compared to traditional methods. One significant advantage is reduced recovery time. Patients often experience faster healing, allowing them to return to their daily lives swiftly. This efficiency can be particularly valuable for those with busy schedules or work commitments.
Another crucial aspect is the precision of MIRS. Surgeons use advanced robotic systems, enhancing their ability to perform intricate procedures. Smaller incisions lead to less tissue damage and lower blood loss. Consequently, patients face a reduced risk of complications. However, the initial learning curve for surgeons adopting this technology can be steep. Training and experience are vital for optimal outcomes.
Patient comfort is an essential factor as well. Many individuals report less pain after minimally invasive procedures. This aspect is often overlooked but can significantly impact a patient’s overall experience. Despite these advantages, not every patient may be a suitable candidate for MIRS. Factors such as medical history and specific conditions should be considered, prompting reflection on the most appropriate approach.
How Robotic Surgery Enhances Precision and Control in Operations
Minimally invasive robotic surgery has transformed how surgeons approach procedures. This technology provides enhanced precision and control, significantly improving patient outcomes. Advanced robotic systems allow for smaller incisions, resulting in reduced postoperative pain and faster recovery times. A study published in the Journal of Robotic Surgery demonstrated that patients undergoing robotic procedures experienced a 30% reduction in hospital stays compared to traditional methods.
The increased dexterity of robotic instruments allows surgeons to perform complex procedures with greater finesse. For instance, studies have shown that robotic-assisted surgeries lead to fewer complications. According to a report from the American College of Surgeons, the complication rate for robotic procedures is about 10% lower than for open surgeries. This increase in precision can decrease blood loss and minimize the risk of infection.
However, the technology is not without challenges. The high cost of robotic surgery can be a barrier for many healthcare systems. Additionally, the learning curve for surgeons to master robotic techniques can lead to variable outcomes. It is vital for institutions to provide comprehensive training and support to ensure the best results for patients. Continuous evaluation of robotic surgery’s impact is necessary to understand its long-term benefits fully.
Patient Recovery: The Role of Less Invasive Options in Healing
Minimally invasive robotic surgery has transformed patient recovery. Research indicates that patients who undergo these procedures often experience shorter hospital stays. A study published in JAMA Surgery shows a reduction in recovery time by 30% compared to traditional methods. This precision leads to less trauma and quicker healing.
The benefits extend beyond hospitalization. Patients report significantly less pain and lower rates of complications. A report from the American College of Surgeons highlights that minimally invasive procedures result in a 50% decrease in post-operative infections. However, this approach isn't without challenges. Surgeons need extensive training to master robotic techniques, and the technology can be costly.
Despite these hurdles, the future looks promising. As surgical technology advances, options for less invasive procedures grow. This evolution offers hope for improved patient outcomes and a more seamless recovery experience. More research is necessary to assess long-term benefits fully. Each patient's condition is unique, and more data can enhance decision-making in surgery.
Outcomes of Minimally Invasive Robotic Surgery vs Traditional Surgery
Comparative Outcomes: Robotic Surgery vs. Traditional Surgical Methods

Robotic surgery has transformed the landscape of medical procedures. It offers precision and minimally invasive techniques that traditional surgeries often cannot match. This approach reduces recovery time and minimizes scarring, which is crucial for many patients. Data shows that patients who undergo robotic procedures experience less postoperative pain compared to traditional methods. This aspect is particularly appealing to those seeking quicker returns to their daily activities.
However, robotic surgery is not without its challenges. Access to such technology can vary by hospital. Not all facilities have the necessary equipment or trained specialists. This can lead to disparities in care. Additionally, some patients may worry about the learning curve associated with robotic techniques. Surgeons must be adequately trained, and some may still prefer established traditional methods for certain procedures.
In considering the right surgical approach, patients should discuss all options. Open communication with healthcare providers is vital. It helps to weigh the benefits of robotic surgery against any potential drawbacks. Individual health circumstances will vary, making personal assessments key to successful outcomes.
Related Posts
-

Why the Robotic Surgery Market is Revolutionizing Healthcare Today
-
What is the Future of Robotic Surgery Market Trends and Opportunities
-
Why Robotic Surgery is Revolutionizing Modern Medicine?
-

How to Understand the Benefits of Minimally Invasive Robotic Surgery?
-

How to Choose the Right Rob Surgical Systems for Your Healthcare Facility?
-

What is the Future of Minimally Invasive Robotic Surgery in 2026?